Denial Management AI
Eliminate 27% of all eligibility and patient data-related denials with Denial management AI.

Go With the Flow With Your Patients!
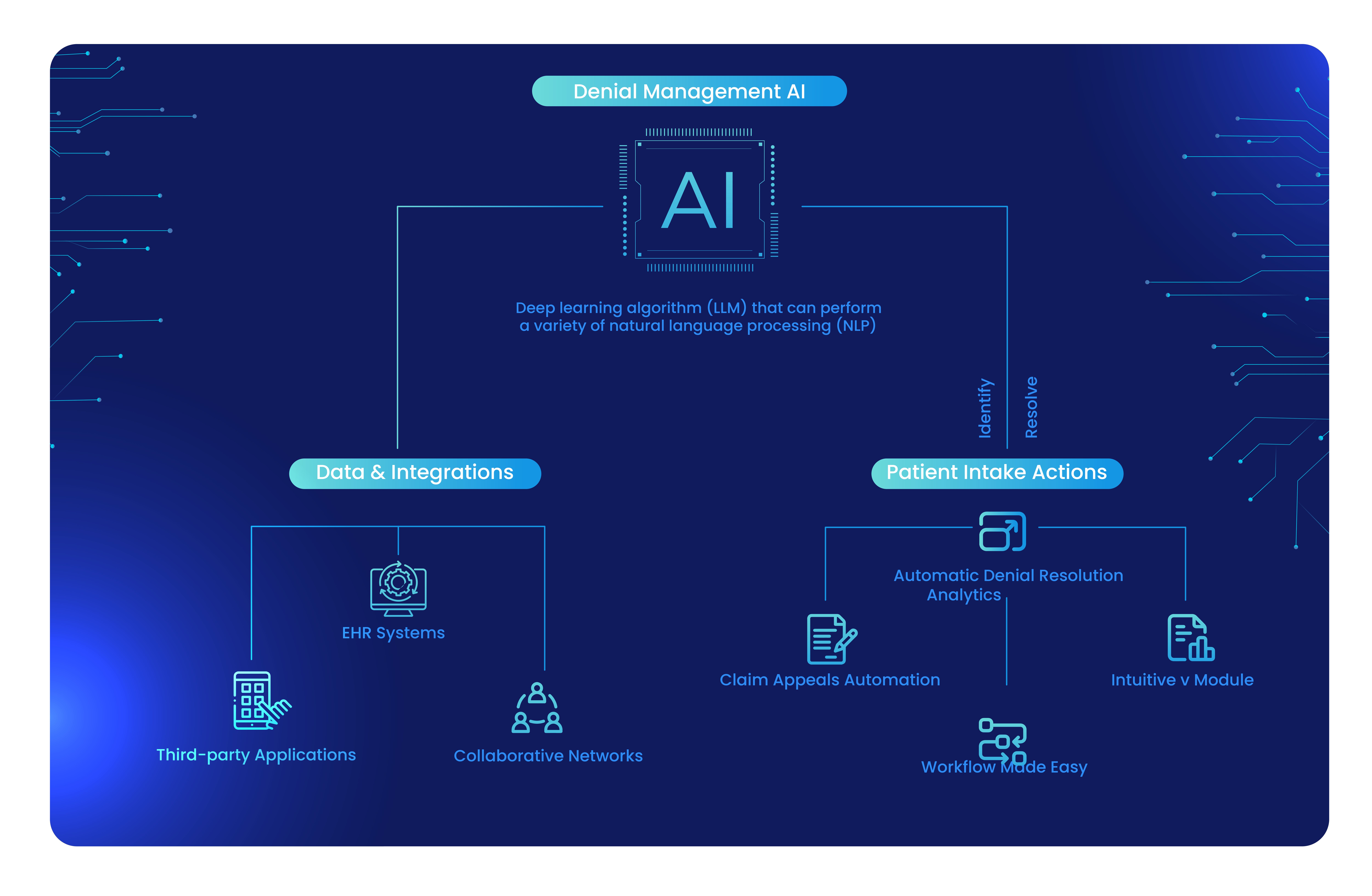
EHR Compatibility
Denial management AI integrates with 60+ major EHRs, ensuring seamless operation with your current system, sans data migration woes.
Workflow Made Easy
If the claim denial requires human intervention the denial management AI assigns to the respective department (coding, AR, credentialing etc.).
Enhance Efficiency
Allow denial management AI to tackle the complexities, enabling front office staff to concentrate on patient care, thereby improving service quality.
HIPAA Assurance
Our denial management AI guarantees total data security, employing PHI protective algorithms in strict compliance with HIPAA, ensuring no data breach risks.
Decreased Denials
Productivity Improvement.
Achieve Net Collections.
Reduced DNFB Accounts.
Search and Destroy Claim Denials
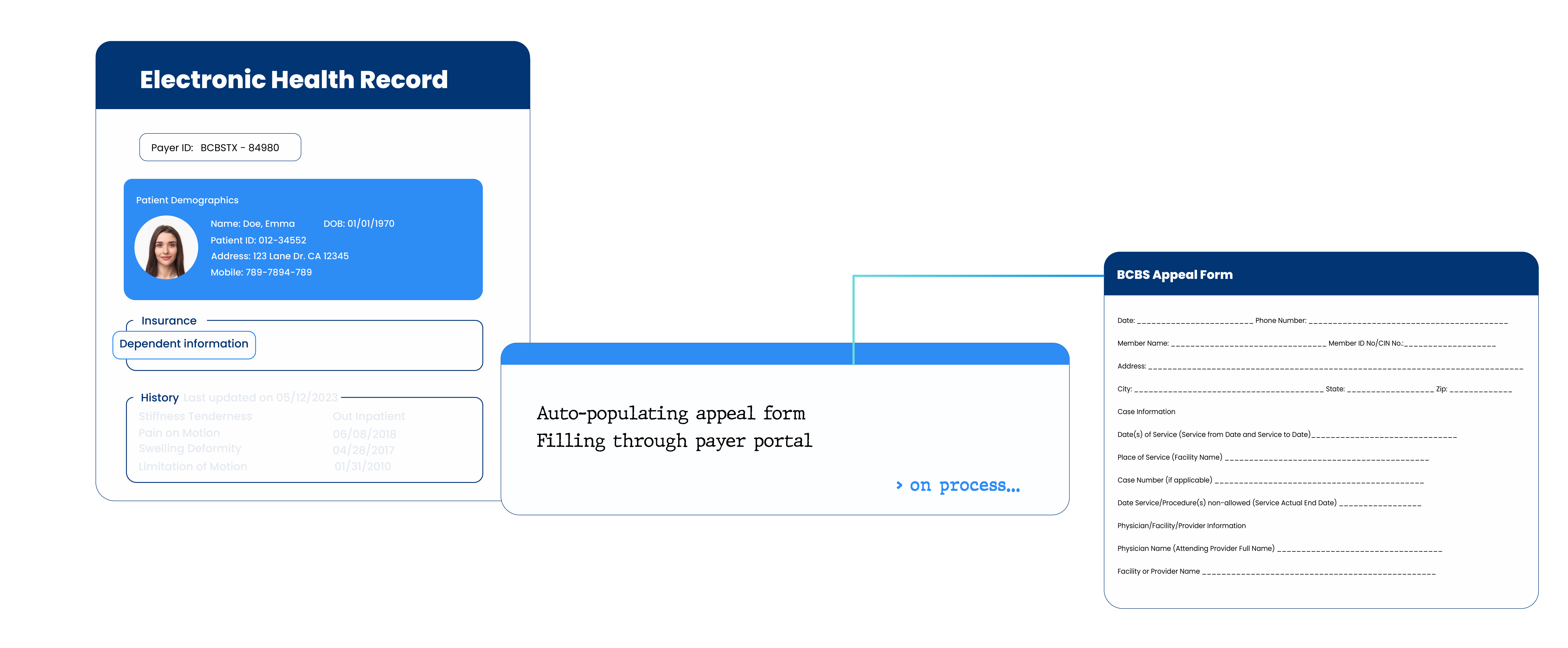
Denial Management AI quickly rectifies insurance verification errors, auto-populating appeal forms and reducing claim rejections for efficient resolution.
Denial Management AI - Solve All Patient Data Centric Claim Denials
Don't let your healthcare organization fall for the 27% of patient data and registration-based denials. Solve with denial management AI.
Automatic Denial Resolution
After grouping eligibility and benefits-related denials denial management AI gathers the necessary information needed for correction and submits the claim automatically.
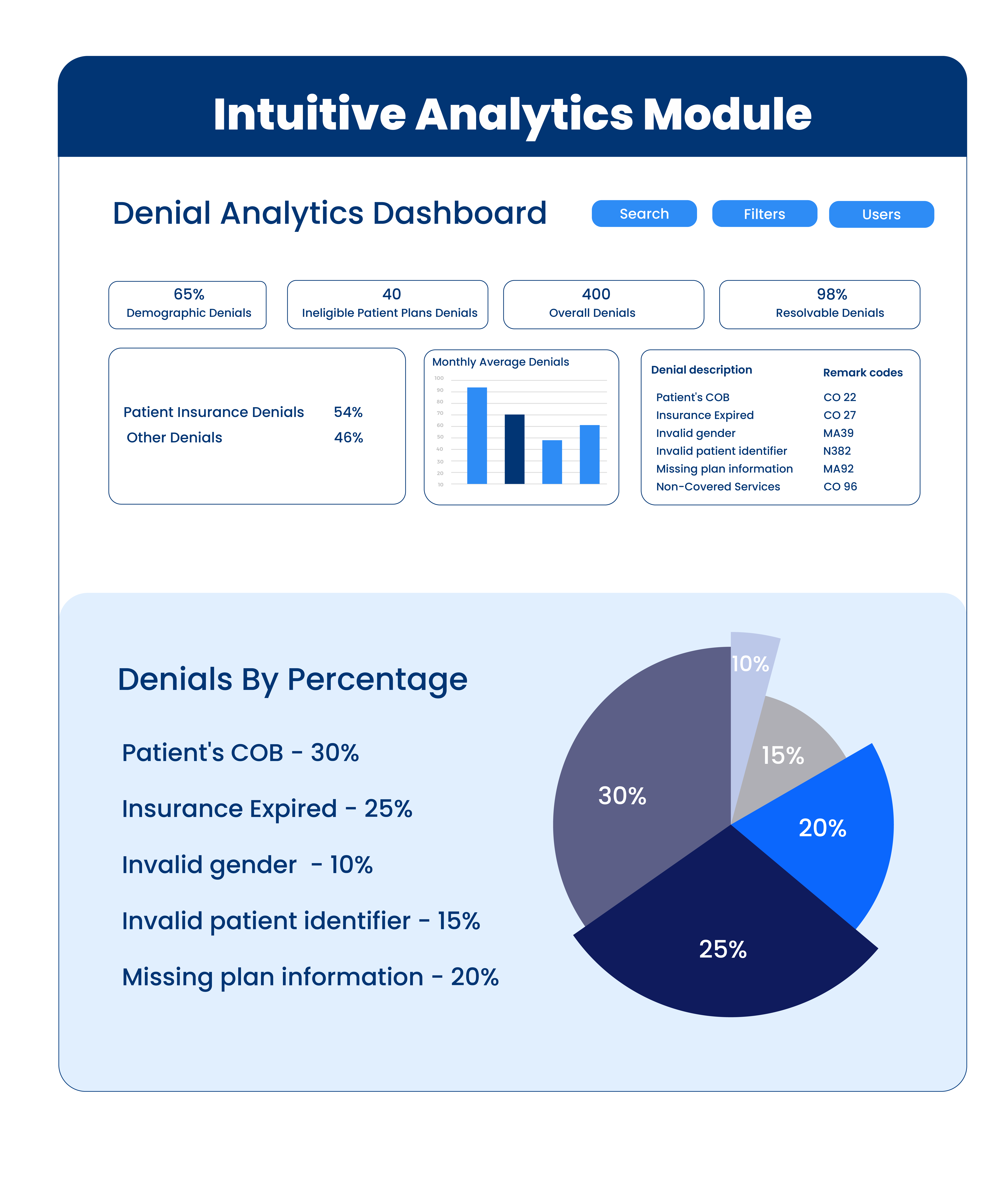
Intuitive Analytics Module
Denial management AI analyzes and identifies patient demographic, eligibility, benefits and non-covered services denials.
Claim Appeals Automation
Find a comprehensive list of payer appeal forms, with the option to upload as needed; denied claim details are auto-filled for convenience.
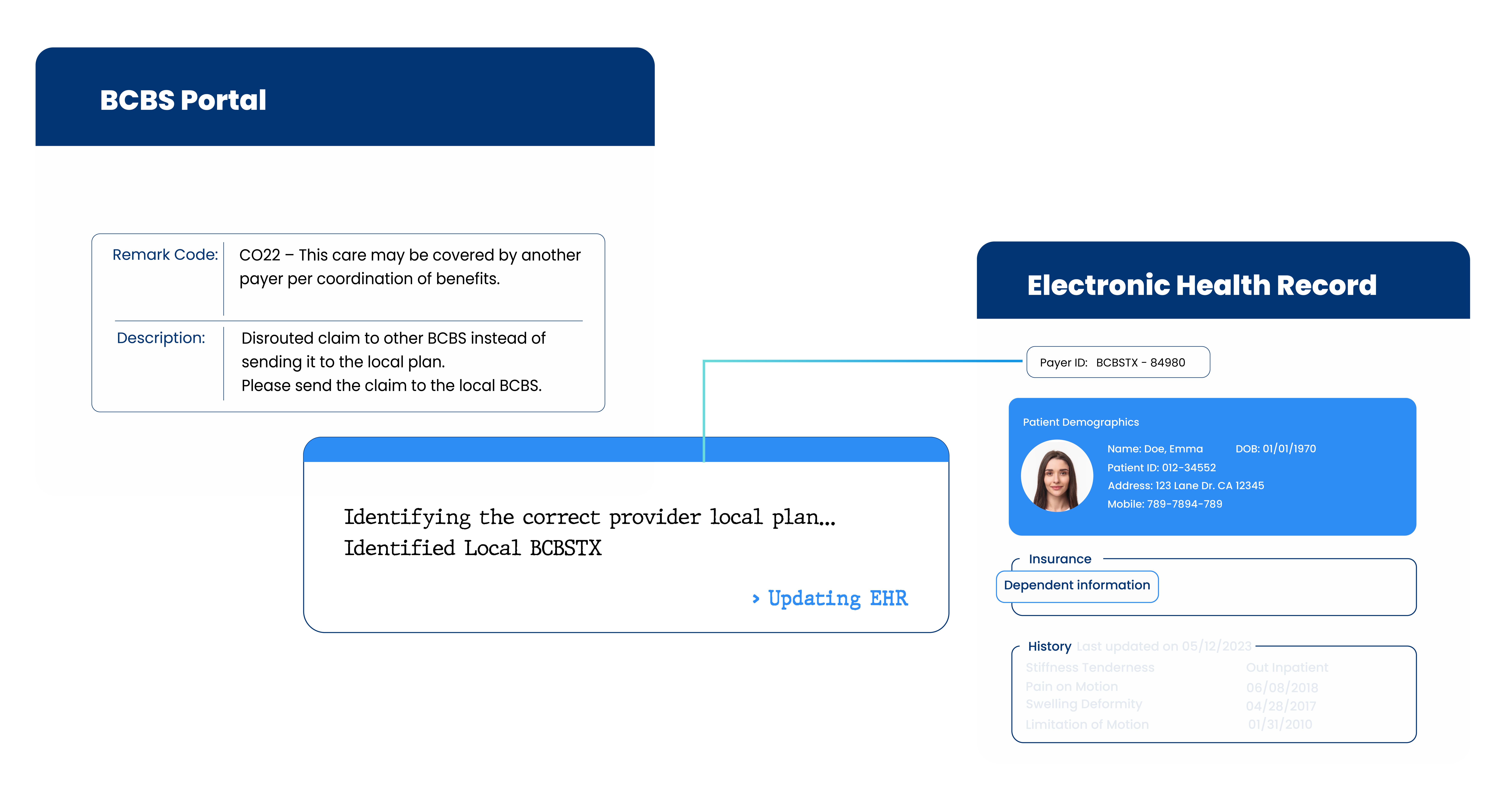
Knockdown demographics and eligibility denials with Denial Management AI
Join us today and experience the power of Patient Intake AI for yourself!